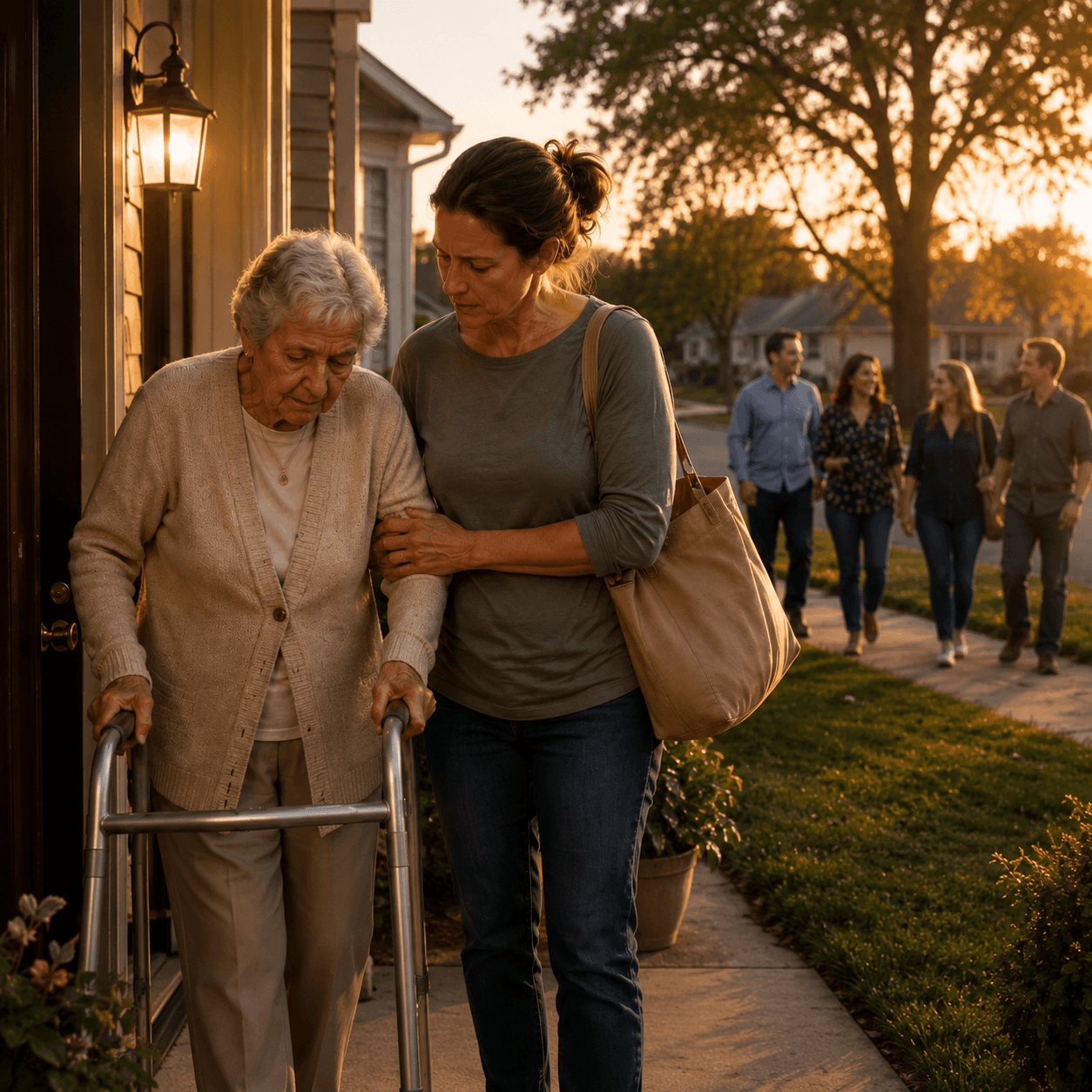
Although caregiving can require you to support your loved one 24/7, it can still feel very lonely at times. Caregiver loneliness can stem from the gap between desired and actual social contact while caring for an older loved one. This experience can easily transform into isolation, where people have limited interactions with family and friends because their caregiving responsibilities are too demanding.
Many caregivers can feel “invisible” because they often have an often thankless job. They can go unnoticed by others, despite being their loved one’s nurse, housekeeper, and advocate.
Caregiver loneliness is a common issue. Research shows that among 23.9 million U.S. caregivers, about 27% reported feeling lonely, and 12% were socially isolated.
If your caregiving responsibilities are making you feel disconnected from the world, know that you can seek help while still caring for your loved one.
Key takeaways
- Caregiver loneliness can develop from a mismatch between how much connection you need and how much you’re able to have.
- Because caregiving can be demanding, it can lead to social isolation and a sense of feeling “invisible,” even when you’re constantly supporting someone.
- You can seek mental health support to improve your well-being without compromising the care you provide.
Coping with the weight of being isolated
Caring for an aging parent or spouse can naturally lead to social isolation. It’s a demanding role that can be emotionally and physically exhausting, with responsibilities ranging from bathing to doctors’ appointments.
If you’re a full-time caregiver, your responsibilities may leave you little time for yourself — and most likely, you’ll use that allotted time to rest. Ultimately, it can be difficult to find time to spend with your family and friends, leading to loneliness and social isolation.
Physical effects of caregiving
Several physical factors can contribute to family caregiver isolation, including:
- Being homebound due to the need for continuous supervision
- Lifting, bathing, or toileting a loved one
- Sleep deprivation occurs when a loved one frequently wakes up at night, has dementia, or requires overnight monitoring
- Caring for a medically fragile loved one
The emotional toll of caregiving
Understandably, caregiving can also be emotionally taxing. Many caregivers may experience anticipatory grief, the profound sadness or anxiety before an impending loss, such as a loved one’s chronic or dementia-related illness.
The person you’re caring for can also experience anticipatory grief, along with sudden mood or personality changes, and the cognitive changes that can come with age-related conditions like dementia or Parkinson’s disease. This can further contribute to emotional distress for caregivers.
The growing social disconnect
In addition to physical and emotional factors that can contribute to the “invisible” caregiver experience, people may also experience strain in their relationships. Friends and family may slowly drift away because they can’t relate to your situation, are uncomfortable, or just assume you’ll reach out to them to hang out.
As much as you love your parent or spouse, it’s important to maintain relationships outside of your caregiving role. When they’re the only person in your circle, it can add to the weight of isolation.
Who’s at risk of caregiver loneliness and invisibility
Spouses and adult children are often the caregivers, and each can have unique risk factors for social isolation and feeling invisible.
For spouse caregiver loneliness, the transition may lead to a decline in the emotional and physical intimacy the couple once shared. It can also create feelings of resentment or grief over the loss of companionship. If their spouse was their main social connection, it can be challenging for them to form new friendships — especially if 24/7 care is required. Research shows that spousal caregivers experience more social isolation than adult caregivers.
Adult children serving as caregivers can also face risks of social isolation. Many fall within the sandwich generation, who are middle-aged adults juggling work while caring for their children and aging parents. Studies show that sandwich generation caregivers can experience physical and emotional strain, possibly leading to depression, social isolation, and loss of social networks.
Having limited or no support can contribute to lonely caregivers. If you’re the only child or live somewhere where you don’t know many people, it can increase the risk of loneliness.
Caring for someone with dementia can be challenging. Caregivers can socially withdraw because of their loved one’s cognitive decline. They may have concerns about their unpredictable behavior, stigma, and anxiety. Dementia caregiving can also be physically and mentally draining, as the condition requires round-the-clock care due to loss of independence, behavioral changes, and safety concerns.
Hidden health costs of caregiver isolation
If caregiver social isolation isn’t addressed with mental health support, it can take a toll on your physical health. Chronic or prolonged loneliness can spike stress hormones, potentially causing inflammation and weakening the immune system. It also increases the risk of heart disease, stroke, type 2 diabetes, dementia, and early death.
Caring for a spouse or aging parent can impact your mental health, too. It can increase your risk of depression, anxiety, as well as burnout — an issue that can affect about 1 in 5 caregivers.
If you feel like an “invisible” caregiver, you may also experience a loss of identity or “role engulfment.” You may believe that you don’t have a life outside of being a caregiver. This can lead to emotional exhaustion, anxiety, and a profound sense of losing yourself.
If caregiving is affecting your physical and mental well-being, know there’s help available to navigate through those issues.
Strategies for coping with loneliness as a caregiver
There are healthy strategies you can adopt to better cope with caregiver isolation. One approach is to redefine your social connections. If attending large gatherings isn’t practical, you can seek out “micro-interactions,” such as brief phone calls or online communities.
Remember that you don’t have to bear all caregiving responsibilities on your own. If you have the financial means, professional home care and adult day centers are available. These support systems can help you reclaim your social life while ensuring your loved one is well-cared for.
How to set boundaries as a caregiver
Even if you’re devoting most of your time to supporting your spouse or aging parent, you still need to prioritize self-care. Setting boundaries can help prevent burnout, reduce stress, and protect your mental and physical health.
Some ways you can set boundaries include:
- Deciding what tasks you can and cannot do, and delegating tasks to others
- Saying “no” without feeling guilty
- Setting specific caregiving hours and including scheduled breaks to rest and recharge
- Reaching out to family members, friends, or professional services for support
It can also be helpful to join support groups to connect with other caregivers who understand what you’re going through. Support groups can provide validation, practical advice, and a sense of belonging.
How Sailor Health can help
Seeking professional help can be a way to address caregiver loneliness. If you’re a Medicare recipient, you have coverage for mental health services for depression, anxiety, and other common conditions. Working with a licensed mental health professional can help you navigate the experience of being a “lonely” caregiver. They can give you the tools to regain a sense of self outside of your caregiving role.
If your loved one is showing signs of mental distress, helping them access Medicare-covered mental health care can not only help them find relief but can also reduce your caregiver burden.
Sailor Health understands the unique experiences of caregivers and makes therapy affordable and accessible. You can access sessions from the comfort of your home online or over the phone, cutting out the need to drive to a therapist’s office. Our therapists are older, experienced, and empathetic, prepared to help you address any mental health struggles you’re facing.
We work with Medicare to cover up to 100% of the cost, and most of our patients have a $0 copay for therapy sessions. Get started today, and you could begin therapy in as little as 24 hours after.
Caregiver loneliness FAQ
Why do I feel so lonely when I am with my parent/spouse all day?
As a caregiver, it’s normal to feel lonely while caring for a spouse or parent. Caregiving can be isolating, leaving little to no time to spend with others.
What is the difference between caregiver loneliness and caregiver burnout?
Caregiver loneliness is a feeling of isolation or disconnection, despite being around others, while caregiver burnout is a state of exhaustion from prolonged, high-stress caregiving responsibilities without adequate support.
Does Medicare cover therapy for family caregivers?
Medicare Part B covers necessary mental health therapy services for beneficiaries, including caregivers 65 and older who qualify for Medicare.
How can I find a support group if I can't leave the house?
If your caregiving responsibilities confine you to your loved one’s home, you can still find support through virtual, in-home, and community-based resources.
Is it normal to feel invisible as a caregiver?
Yes, it is completely normal to feel invisible as a caregiver. This experience can stem from social isolation and a lack of support.
References
- Qian, Y., Pomeroy, M. L., Petchler, C. M., Saylor, M. A., Cudjoe, T. K. M., & Ornstein, K. A. (2025). The Epidemiology of Social isolation and loneliness among family and unpaid caregivers of Older adults: Findings from the National Study of CareGiving. The Journals of Gerontology Series B, 80(7). https://academic.oup.com/psychsocgerontology/article-abstract/80/7/gbaf101/8145524
- Li, L., Wister, A. V., & Mitchell, B. (2020). Social isolation among Spousal and Adult-Child Caregivers: Findings from the Canadian Longitudinal Study on Aging. The Journals of Gerontology Series B, 76(7), 1415–1429. https://pmc.ncbi.nlm.nih.gov/articles/PMC8363033/
- Pashazade, H., Maarefvand, M., Momtaz, Y. A., & Abdi, K. (2024). Coping strategies of the sandwich generation in the care process: a qualitative study. BMC Public Health, 24(1), 3373. https://pmc.ncbi.nlm.nih.gov/articles/PMC11616165/#
- Health effects of social isolation and loneliness. (2024, May 15). Social Connection. https://www.cdc.gov/social-connectedness/risk-factors/index.html
- Soh, X. C., Hartanto, A., Ling, N., Reyes, M., Sim, L., & Majeed, N. M. (2025). Prevalence of depression, anxiety, burden, burnout, and stress in informal caregivers: An umbrella review of meta-analyses. Archives of Gerontology and Geriatrics Plus, 2(3), 100197. https://www.sciencedirect.com/science/article/pii/S2950307825000785
Frequently Asked Questions
What is Sailor Health?

Sailor Health is a premium mental health service designed specifically for older adults. We connect seniors with licensed therapists who specialize in geriatric care, offering personalized therapy to address issues like anxiety, depression, and the challenges of aging.
Our services are accessible through secure online or phone-based sessions, making it easy for those to receive care from the comfort of their own homes.
Is Sailor Health covered by insurance?

Yes, Sailor Health is in-network with Medicare, making our services accessible and affordable for our clients. We believe that mental health care should be within reach for everyone, so we work hard to ensure that our services are affordable but exceptional.
What if my loved one isn’t comfortable with technology?

We understand that technology can be intimidating for some older adults. Studies show that many older adults actually find online therapy more comfortable and convenient once they try it, with clinical outcomes comparable to in-person therapy.
Seniors can join therapy sessions with a simple video link or a phone call (no smart phone required). We offer step-by-step guidance and are available to help with any technical issues, ensuring that technology doesn’t stand in the way of receiving quality therapy.
How do I know if a therapist is the right fit for me?

We carefully match you with a therapist based on your preferences and needs. To help you feel confident in your choice, we offer a consultation to discuss your goals and preferences. If it’s not the right fit, we’ll work with you to find a therapist who is.
How do you ensure privacy and confidentiality?

Privacy and confidentiality are cornerstones of our service at Sailor Health. We use secure, HIPAA-compliant platforms for all telehealth sessions, ensuring that your personal information and the details of your therapy are kept strictly confidential. Our therapists adhere to professional ethical standards, and we have rigorous data protection measures in place to safeguard your privacy at all times.
About the author

Taneia Surles

%20(390%20x%20424%20px).avif)


.avif)
%20(390%20x%20424%20px)%20(400%20x%20400%20px).avif)
%20(390%20x%20424%20px)%20(400%20x%20400%20px).avif)

%20(390%20x%20424%20px)%20(400%20x%20400%20px).avif)
%20(390%20x%20424%20px).avif)






